Took Bp Reading 3 Imes First Was Higher Than Oyhers
Blood pressure may be the vital sign we measure the nigh and empathize the to the lowest degree
Nurses and physicians often argue over differences between arterial line and not-invasive blood pressure (NIBP) cuff readings. Revised guidelines for management of high blood pressure level increased thresholds for diagnosing and treating hypertension, causing further argue and controvery [1].
To brand the best use of blood force per unit area monitoring equipment, it is helpful to have an insight into how the equipment works and the likely sources of mistake that can affect readings. Download a guide to these tips to keep with you for quick reference.
The about mutual claret pressure reading mistakes are:
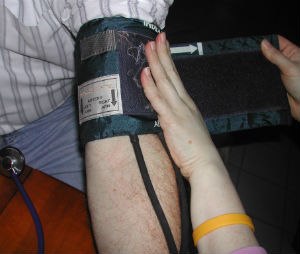
- Using the wrong-sized cuff
- Wrong patient positioning
- Wrong cuff placement
- Normal reading prejudice
- Non factoring in electronic units correctly
Here's what many of us do wrong, and how to take a blood pressure level reading:
1. You're using the wrong-sized cuff
The almost common mistake when using indirect blood pressure measuring equipment is using an incorrectly sized cuff. A BP cuff that is too large will give falsely low readings, while an overly small gage volition provide readings that are falsely high.
The American Heart Association publishes guidelines for claret force per unit area measurement [2]. recommending that the bladder length and width (the inflatable portion of the cuff) should be 80 pct and twoscore percent respectively, of arm circumference. Virtually practitioners find measuring float and arm circumference to exist overly fourth dimension consuming, so they don't practice it.
The most applied way to speedily and properly size a BP cuff is to pick a gage that covers 2-thirds of the distance between your patient'southward elbow and shoulder. Carrying at to the lowest degree 3 cuff sizes (big adult, regular adult, and pediatric) will fit the majority of the developed population. Multiple smaller sizes are needed if you ofttimes care for pediatric patients.
Korotkoff sounds are the noises heard through a stethoscope during cuff deflation. They occur in 5 phases:
- I – first detectable sounds, corresponding to appearance of a palpable pulse
- Two – sounds become softer, longer and may occasionally transiently disappear
- Three – change in sounds to a thumping quality (loudest)
- 4 – pitch intensity changes and sounds become deadened
- V – sounds disappear
In their 1967 guidelines, the AHA recommended that clinicians record the systolic BP at the start of phase I and the diastolic BP at start of phase IV Korotkoff sounds. In their 1981 guidelines, the diastolic BP recommendation changed to the start of phase 5 [2].
two. You lot've incorrectly positioned your patient's trunk
The 2d most common fault in BP measurement is incorrect limb position. To accurately assess blood menses in an extremity, influences of gravity must be eliminated.
The standard reference level for measurement of blood pressure level by whatsoever technique — direct or indirect — is at the level of the middle. When using a gage, the arm (or leg) where the gage is practical must be at mid-heart level. Measuring BP in an extremity positioned above heart level will provide a falsely low BP whereas falsely loftier readings will be obtained whenever a limb is positioned below heart level. Errors can be meaning — typically ii mmHg for each inch the extremity is above or below heart level.
A seated upright position provides the most authentic blood pressure, as long equally the arm in which the force per unit area is taken remains at the patient'southward side. Patients lying on their side, or in other positions, can pose problems for authentic pressure measurement. To correctly assess BP in a side lying patient, agree the BP cuff extremity at mid heart level while taking the pressure level. In seated patients, exist sure to leave the arm at the patient's side.
Arterial pressure transducers are subject to similar inaccuracies when the transducer is not positioned at mid-middle level. This location, referred to equally the phlebostatic centrality, is located at the intersection of the quaternary intercostal space and mid-chest level (halfway between the inductive and posterior chest surfaces.
Notation that the mid-axillary line is oft not at mid-chest level in patients with kyphosis or COPD, and therefore should non be used equally a landmark. Incorrect leveling is the primary source of error in direct force per unit area measurement with each inch the transducer is misleveled causing a 1.86 mmHg measurement error. When above the phlebostatic axis, reported values will be lower than actual; when beneath the phlebostatic axis, reported values will exist college than actual.
three. You've placed the cuff incorrectly
The standard for blood pressure cuff placement is the upper arm using a cuff on blank skin with a stethoscope placed at the elbow fold over the brachial artery.
The patient should be sitting, with the arm supported at mid heart level, legs uncrossed, and non talking. Measurements can be made at other locations such equally the wrist, fingers, anxiety, and calves but will produce varied readings depending on distance from the centre.
The mean pressure, interestingly, varies picayune betwixt the aorta and peripheral arteries, while the systolic force per unit area increases and the diastolic decreases in the more than distal vessels.
Crossing the legs increases systolic blood pressure by 2 to 8 mm Hg. About 20 percent of the population has differences of more than than 10 mmHg pressure between the correct and left arms. In cases where meaning differences are observed, treatment decisions should be based on the college of the 2 pressures.
4. Your readings exhibit 'prejudice'
Prejudice for normal readings significantly contributes to inaccuracies in blood force per unit area measurement. No doubt, you'd be suspicious if a boyfriend EMT reported blood pressures of 120/eighty on three patients in a row. Equally creatures of habit, human beings wait to hear sounds at certain times and when extraneous interference makes a blood pressure difficult to obtain, at that place is considerable trend to "hear" a normal blood pressure.
Orthostatic hypotension is defined every bit a decrease in systolic claret pressure of 20 mm Hg or more, or diastolic claret pressure level decrease of 10 mm Hg or more measured afterward 3 minutes of standing quietly.
There are circumstances when BP measurement is only non possible. For many years, trauma resuscitation guidelines taught that rough estimates of systolic BP (SBP) could exist made by assessing pulses. Presence of a radial pulse was idea to correlate with an SBP of at least 80 mm Hg, a femoral pulse with an SBP of at to the lowest degree seventy, and a palpable carotid pulse with an SBP over 60. In recent years, vascular surgery and trauma studies have shown this method to be poorly predictive of actual blood pressure [iii].
Racket is a factor that tin too interfere with BP measurement. Many ALS units carry doppler units that measure claret flow with ultrasound waves. Doppler units amplify sound and are useful in high noise environments.
BP by palpation or obtaining the systolic value by palpating a distal pulse while deflating the blood pressure cuff generally comes within 10 – 20 mmHg of an auscultated reading. A pulse oximeter waveform tin can also exist used to mensurate return of blood flow while deflating a BP cuff, and is as accurate as pressures obtained by palpation.
In patients with circulatory assist devices that produce non-pulsatile flow such as left ventricular assist devices (LVADs), the only indirect means of measuring menses requires use of a doppler.
The return of flow signals over the brachial artery during deflation of a blood pressure cuff in an LVAD patient signifies the mean arterial pressure (MAP). While a normal MAP in adults ranges from seventy to 105 mmHg, LVADs do not function optimally against higher afterload, then mean pressures of less than ninety are oftentimes desirable.
Clothing, patient admission, and cuff size are obstacles that frequently interfere with conventional BP measurement. Consider using alternate sites such equally placing the BP cuff on your patient's lower arm above the wrist while auscultating or palpating their radial artery. This is peculiarly useful in bariatric patients when an appropriately sized cuff is not available for the upper arm. The thigh or lower leg can be used in a similar fashion (in conjunction with a pulse point distal to the gage).
All of these locations are routinely used to monitor BP in hospital settings and generally provide results only slightly dissimilar from traditional measurements in the upper arm.
five. You're not factoring in electronic units correctly
Electronic blood pressure units also called Not Invasive Blood Pressure level (NIBP) machines, sense air pressure level changes in the cuff caused by claret flowing through the BP cuff extremity. Sensors estimate the Mean Arterial Pressure level (MAP) and the patient'due south pulse charge per unit. Software in the car uses these two values to summate the systolic and diastolic BP.
To assure accuracy from electronic units, it is important to verify the displayed pulse with an actual patient pulse. Differences of more than 10 percent volition seriously modify the unit of measurement's calculations and produce wrong systolic and diastolic values on the display screen.
Given that MAP is the only pressure actually measured by an NIBP, and since MAP varies little throughout the body, information technology makes sense to utilise this number for treatment decisions.
A normal adult MAP ranges from 70 to 105 mmHg. As the organ most sensitive to pressure, the kidneys typically require an MAP above threescore to stay alive, and sustain irreversible damage beyond twenty minutes below that in near adults. Because individual requirements vary, most clinicians consider a MAP of 70 as a reasonable lower limit for their adult patients.
Increased use of NIBP devices, coupled with recognition that their displayed systolic and diastolic values are calculated while simply the hateful is actually measured, have led clinicians to pay much more than attention to MAPs than in the past. Many progressive hospitals order sets and prehospital BLS and ALS protocols have begun to care for MAPs rather than systolic blood pressures.
Finally, and especially in the critical intendance ship environment, providers volition meet patients with significant variations betwixt NIBP (indirect) and arterial line (directly) measured blood force per unit area values.
In the past, depending on patient condition, providers take elected to use one measuring device over another, ofttimes without articulate rationale besides a belief that the selected device was providing more authentic blood pressure level information.
In 2013, a grouping of ICU researchers published an analysis of 27,022 simultaneous art line and NIBP measurements obtained in 852 patients [iv]. When comparing the a-line and NIBP readings, the researchers were able to determine that, in hypotensive states, the NIBP significant overestimated the systolic blood pressure when compared to the arterial line, and this difference increased as patients became more hypotensive.
At the same fourth dimension, the mean arterial pressures (MAPs) consistently correlated between the a-line and NIBP devices, regardless of pressure. The authors suggested that MAP is the most accurate value to trend and treat, regardless of whether BP is beingness measured with an arterial line or an NIBP. Additionally, supporting previously believed parameters for acute kidney injury (AKI) and mortality, the authors noted that a MAP beneath lx mmHg was consistently associated with both AKI and increased mortality.
Since 1930, blood pressure measurement has been a widely accepted tool for cardiovascular cess. Even under the oft adverse conditions encountered in the prehospital or send environment, providers can accurately measure blood force per unit area if they understand the principles of blood flow and common sources that introduce error into the measurement process.
Blood pressure assessment tips
Keep learning most blood pressure level assessment by reading how to mitigate NIBP and auscultating innacuracies by watching the plethysmography waveform on your pulse oximeter and noting the mean arterial pressure.
Read side by side: Acquire how to read a MAP.
References:
one. James PA, Oparil S, Carter BL, et al. 2014 Evidence-Based Guideline for the Direction of Loftier Blood Pressure in Adults: Report From the Panel Members Appointed to the Eighth Joint National Committee (JNC eight). JAMA. 2014;311(5):507-520. (Available at: http://jama.jamanetwork.com/article.aspx?articleid=1791497)
two. Pickering TG, Hall JE, Appel LJ, et al. AHA Scientific Argument: Recommendations for claret pressure level measurement in humans and experimental animals, part 1: claret pressure level measurement in humans. Hypertension. 2005; 45: 142-161. (Bachelor at: https://hyper.ahajournals.org/content/45/i/142.full)
3. Deakin CD, Low JL. Accurateness of the advanced trauma life back up guidelines for predicting systolic blood pressure level using carotid, femoral, and radial pulses: observational study. BMJ. 2000; 321(7262): 673–674. (Available at: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC27481/)
4. Lehman LH, Saeed Yard, Talmor D, Mark R, Malhotra A. Methods of blood pressure level measurement in the ICU. Crit Care Med. 2013;41:34-xl.
This article, originally posted Apr. 9, 2014, has been updated.
Fill out the grade beneath to download a guide to reading blood pressure.
Well-nigh the writer
Mike McEvoy, PhD, NRP, RN, CCRN is the EMS Coordinator for Saratoga Canton, New York and a paramedic supervisor with Clifton Park & Halfmoon Ambulance. He is a nurse clinician in cardiothoracic surgical intensive intendance at Albany Medical Center where he as well Chairs the Resuscitation Committee and teaches disquisitional care medicine. He is a lead author of the "Critical Care Transport" textbook and Informed® Emergency & Critical Care guides published by Jones & Bartlett Learning. Mike is a contributor to EMS1.com and a popular speaker at European monetary system, Burn, and medical conferences worldwide. Contact Mike by electronic mail.
whickereversheyea.blogspot.com
Source: https://www.ems1.com/ems-products/medical-monitoring/articles/5-errors-that-are-giving-you-incorrect-blood-pressure-readings-zJNOHnFJZOocufoS/
0 Response to "Took Bp Reading 3 Imes First Was Higher Than Oyhers"
Post a Comment